Check out our latest blog article: From component to enterprise – modular robotics done right.
Rethinking Remote Patient Monitoring in 2020

Over the years, remote patient monitoring (RPM) has been seen as a powerful new technology, which will reshape healthcare as we know it—somewhere in the distant future. The unprecedented challenges of the COVID-19 pandemic, however, have completely altered the telehealth landscape and the way patients receive healthcare services. Today, the healthcare industry urgently needs new technology tools to extend the reach of physicians and support the monitoring of infected, recovered, and discharged patients.
To help healthcare CIOs, CMOs, and other leaders adjust the way they deliver care with RPM and wearables, here are some key facts about RPM technology and the ways it can be employed.
RPM Implementation Prior to and During COVID-19
As part of the broader telehealth concept, RPM has received much attention and praise from healthcare professionals (HCPs) and patients alike. Back in November 2019, 88% of healthcare providers were already investing in RPM systems. There were multiple reasons behind it:
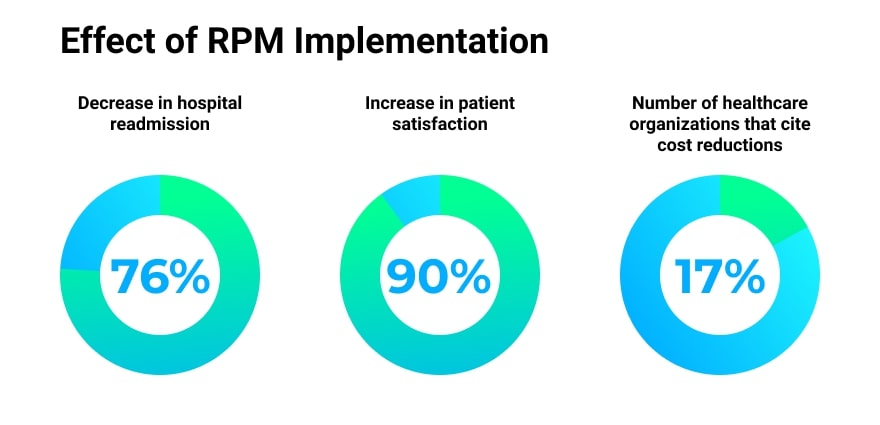
- Reduction in hospital readmission and clinical visits. By equipping patients with tablets and RPM equipment, the University of Pittsburgh Medical Center reduced the risk of hospital readmissions by 76%, while boosting patient satisfaction scores by over 90%.
- Positive ROI from RPM technology and home-based care. According to the KLAS Research report, 17% of healthcare organizations running RPM programs cited cost reductions.
- Timely informed advice and feedback. RPM solutions ensure 24/7 monitoring that allows for adjusting treatment, dosages, and medical recommendations, falling in line with the global trend towards patient centricity. The system also supports clinicians to make informed, timely care decisions.
- A more comprehensive picture of a patient’s status. Wearables, smartphones, and home monitors provide access to huge volumes of data. According to the Stanford Medicine paper on Harnessing the Power of Data in Healthcare, “[a] focus on data in the coming years has the potential to make healthcare more preventive, predictive and personalized, and meaningfully reduce health care costs and lead to better patient care.”
With the COVID-19 outbreak, the world has changed beyond recognition. The long-discussed remote care has seen more progress in the last two months than in preceding years.
The healthcare industry in every country is facing a multifaceted challenge. Today, HCPs need to advise and treat patients with suspected and confirmed cases of COVID-19, provide tailored treatment recommendations, and ensure continuous patient care, when the HCP and hospital access is highly restricted.
Remote care options help preserve healthcare system capacity for COVID-19 patients in a number of ways:
- Decreasing the risk of virus transmission among patients, community members, and healthcare workers
- Providing timely hospital-based care or helping patients recover at home while avoiding hospital bed shortage
- Getting qualitative measurements of patient’s health status and disease progression
- Sending notifications to hospital staff to prepare for COVID-19 patients’ arrival
However, most healthcare providers are facing one of the following issues:
- Absence of a remote-working crisis response plan. Healthcare providers that previously relied solely on hospital facilities are struggling to handle the increasing number of patients.
- Lack of infrastructure supporting remote patient care. In many instances, HCPs possess elements of the RPM architecture, such as wearable devices for patient monitoring. But they are lacking other components, like a provider interface or delivery mechanisms, and need to make quick improvements to align the existing RPM solution with today’s clinical needs.
- Technical challenges. Troubles with network reliability, user errors, and power consumption of the RPM solution in place.
Healthcare providers are now investigating the opportunities to merge novel RPM tools into their existing IT infrastructures and adapt their legacy systems and databases to the new environment.
How Does an RPM Solution Function?
According to the Center for Connected Health Policy, “remote patient monitoring uses digital technologies to collect medical and other forms of health data from individuals in one location and electronically transmit that information securely to health care providers in a different location for assessment and recommendations”.
Today, there are multiple RPM systems on the market, which differ in shape, purpose, and features:
- Voice apps, such as Dexcom’s continuous glucose monitors (CGMs), that send notifications to diabetes patients, alerting them to take their insulin
- Blood pressure cuffs, which transmit blood pressure and pulse data to physicians
- Wearable patches, like Vital Scout, which features ECG sensors to measure stress and recovery rates
Regardless of the functionality and form factor, they all are based on the same technology that collects and interprets physiologic data.
RPM solutions rely on several technology components. These include Body Area Networks (BANs), back-end systems, and user interfaces.
- BANs monitor vital signs parameters with the help of sensors and actuators: pulse rate, blood pressure, core temperature, ECG, etc. A healthcare BAN application may be comprised of implants, or invasive devices, for example, implantable cardiac defibrillators (ICDs), and wearable health devices (WHDs), worn on or around the body: smartwatches, ear devices, chest straps, adhesive patches, and many others.
BAN devices use wired, wireless, or hybrid networks to exchange data and communicate with each other. Connected into a single network, the BAN enables local data processing for real-time feedback and centralization of data in a Portable Unit.
- Portable Unit (PU). Implemented on a smartphone or another handheld mobile device, a PU receives analog vital signs, amplifies and filters the signals, and converts raw biosignal data into digital signals. Other functions include data processing and local storage on an edge device.
- Back-end system. A remote central server is the central component of the RPM architecture. It provides services for storing, accessing, and analyzing the biosignals collected within the RPM system, along with data from other sources, such as EHR/EMR, and analytic systems.
- Diagnostic application software. Synchronized with the BAN, it visualises the collected biosignals and provides clinical staff, healthcare experts, and patients with easy access to real-time data. The software is generally comprised of web-based and mobile application components. The system sends an alarm message to HCPs, when the measured data exceeds the allowable normal range.
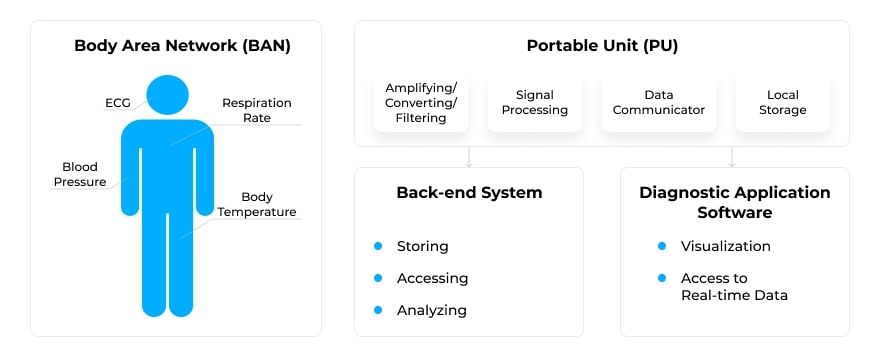
Connected into a single RPM system, these elements ensure real-time monitoring outside a medical facility, alerting both the medical staff and the patient in case of any physiological problem or emergency.

Major Trends in the RPM Market in 2020
A growing interest in RPM systems is a sign of the inevitable trend towards the decentralization of care delivery.
As a result, we are witnessing an exponential increase in the number of RPM projects and wearable devices along with a decrease in the quantity of in-hospital devices and equipment. The COVID-19 pandemic is accelerating time to market, serving as a catalyst to global changes in the healthcare industry.
In the upcoming months, the following trends are likely to emerge:
- A shift towards sensors “made for wearables”. To be efficient, remote patient monitoring requires more accurate sensors. Sensors, targeted specifically for the healthcare industry, will be stable, resilient, and biocompatible.
- Wearable devices capturing medical-grade data. New sensors allow device manufacturers and original equipment manufacturers (OEMs) to distinguish consumer electronics and medical devices, like Apple did when it launched its ECG Watch. Medical-grade devices provide higher quality monitoring functionality and need pre-market approval from the US Food and Drug Administration (FDA), the European Medicines Agency (EMA), and other regulatory bodies.
- Device miniaturization. To increase the functionality and portability of WHD, device makers will be making RPM devices smaller and less invasive, while keeping them power-efficient.
- Deployment of new communication strategies. The global rollout of 5G will significantly influence the communication protocols landscape in wearables-based RPM systems. The major contribution of 5G will be the unprecedented speed with which users can remotely access a BAN. The 5G structure will be able to support the cryptographic solutions necessary to transmit the sheer quantity of data that must be securely sent in real-time to make a BAN function as it is intended.
Like any other crisis, the COVID-19 pandemic can become an opportunity to unlock the potential of the new RPM technology and accelerate its implementation and market growth.
More articles on the topic



![[Webinar] T-Winning Strategies: How Digital Twins Drive Innovation & Efficiency](https://www.softeq.com/hubfs/Digital%20Twins%20Webinar.png)
![[Webinar] Wearables: Past, Present, & Future](https://www.softeq.com/hubfs/Blog%20Featured%20Image.png)

